Bella – A Persistant Cough
Name: Bella
Age: 8yrs old
Weight: 5kg
Breed: Shih Tzu x Schnauzer
Sex: Female, desexed
History: Little Bella is a gorgeous 8yr old Shih Tzu X Schnauzer who came to see Dr Nichola as her family was concerned that she had been coughing for a few days. Bella’s family noticed her breathing sounded quite snuffly and wheezy, but she still seemed bright and happy. Bella had exhibited intermittent coughing episodes in the past, but this time her mum was concerned as the coughing was quite frequent and it had started after Bella had been given some cooked bones. There was a risk that Bella could have had a bone caught in her upper airways or oesophagus.
Examination: On Physical examination, Bella indeed appeared bright and happy but her breathing sounded louder than normal in both her upper respiratory tract (trachea, larynx, mouth, nose) and her lower respiratory tract (lungs). Dr Nichola was concerned that Bella also had a significant heart murmur which was loudest over the left side of her heart. Heart murmurs are typically indicative of increased blood turbulence within the major valves of the heart. A left sided heart murmur is commonly seen with ‘mitral valve’ dysplasia. The mitral valve is like a one way tap that separates the left atrium from the left ventricle. Blood should only move forwards when the valve is healthy. When this valve becomes thickened, blood moves backwards as well as forwards through the valve (regurgitation). A “swooshing” sound, or murmur, is heard when listening with the stethoscope over the affected area. This condition is common in smaller, older dogs.
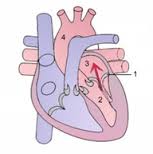
The above diagram explains Mitral Regurgitation. During sytole (when the heart beats), contraction of the left ventricle causes abnormal backflow (refer to the arrow in the diagram) into the left atrium. In the diagram, number 1 shows the Mitral Valve, Number 2 is the Left Ventricle, number 3 is the Left Atrium and number 4 is the Aorta.
Dogs with left sided murmurs and mitral valve disease are at risk of developing ‘congestive heart failure’ which is characterised by fluid accumulation on the lungs (pulmonary oedema). This occurs due to the heart muscle weakening and becoming less effective at pumping blood around the body. Pulmonary oedema develops due to an increase in pressure in the pulmonary (lung) vessels due to the impediment of blood returning from the lungs to the heart. Pulmonary oedema is a medical emergency and potentially life threatening condition as it prevents the normal oxygenation of the blood and dogs become ‘hypoxic’ (low blood oxygen). The best way to diagnose pulmonary oedema is to take chest x-rays and look for an increase in the ‘whiteness’ of the lungs (normal lungs should look almost black on x-rays).
Dr Nichola decided that x-rays needed to be done straight away so that treatment for congestive heart failure could be started if necessary. The x-rays would also highlight any lodged bones if they were present.

The x-ray above shows a dog with pulmonary oeda (fluid on the lungs). The lungs look whiter than normal.
Treatment: Bella was admitted to hospital straight away and x-rays performed. Thankfully there was no evidence of any lodged bones. Bella did have some changes to her lungs on the x-rays but Dr Nichola was not convinced that the changes were consistent with pulmonary oedema. Dr Nichola thought the changes were more consistent with airway (lung) disease, despite her heart murmur.
An appointment was made with the specialist veterinary cardiologist Dr Brad Gavaghan for the following morning to investigate the heart murmur. Bella was discharged from Wilston Vet with doxycycline antibiotics for a possible upper respiratory tract infection. It is important to monitor dogs with cardiac disease closely so Bella was to be taken straight to an emergency after-hours vet if she looked like she was struggling to breath or if her resting respiratory rate was more than 30 breaths per minute (this could indicate pulmonary oedema and impending heart failure).
Dr Gavaghan examined Bella and agreed that she had a significant heart murmur. An ultrasound of her heart (an echocardiogram) show moderate mitral regurgitation and chronic degenerative mitral valve disease. He agreed that her lungs did not look completely normal on her x-rays but the changes were not consistent with pulmonary oedema due to heart disease. Given Bella’s history and physical examination, Dr Gavaghan concurred with Dr Nichola that chronic airway disease (trachea-bronchitis) was the main cause of her cough.
Treatment recommendations for the heart murmur included avoiding strenuous exercise and high salt diets. Dr Gavaghan predicted that Bella is unlikely to experience congestive heart failure within the next 1-2 years. A repeat echocardiogram was recommended to be performed in 12 months to give a more accurate guide to the rate of her heart disease. In the interim, Bella did not require any medications.
Bella’s cough has improved with the antibiotics but her breathing is still a bit noisy. Dr Gavaghan did not recommend any inhalers (e.g. Ventolin) for her bronchitis as her cough is not affecting her quality of life and these medications can have side-effects on the heart. Bella is a much loved member of the family and she will be closely monitored for any possible worsening of her respiratory disease in the future.


